Fibroids, Fertility, and Pregnancy

Get the low-down on fibroids and what they mean for getting pregnant. Q&A with Dr. Naz. You asked, she answered.
What are fibroids?
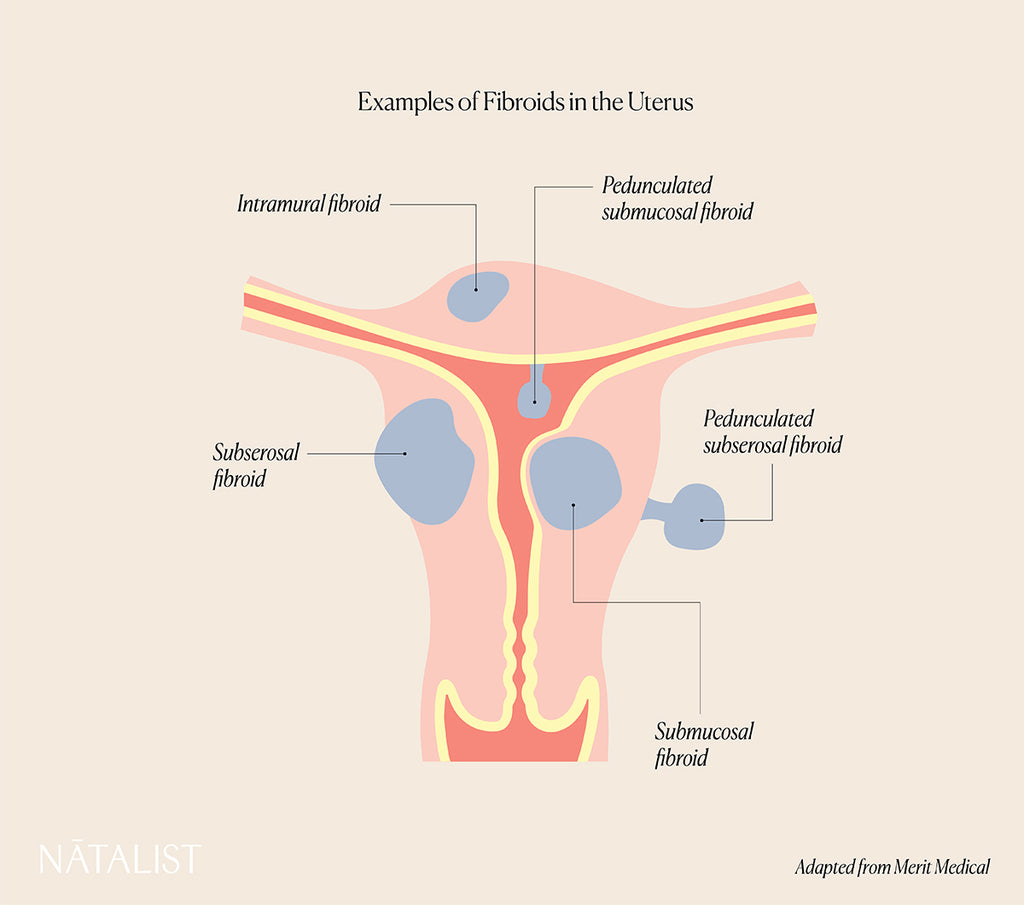
Fibroids are the most common benign (noncancerous) pelvic tumors in women and are commonly referred to as leiomyomas or myomas in medical lingo. OBGYNs characterize fibroids based on their location. They can be:
- Submucosal: within the inner lining of the uterus (called the endometrium)
- Intramural/transmural: spanning the middle lining of the uterus
- Subserosal: right under the outer layer of the uterus
- Pedunculated: coming off the exterior uterus, cervix, or broad ligament with a stalk
A population based study in the U.S. detected fibroids in 59% of black women and 43% of white women. For women in their late 40s, the estimated frequency of fibroids was >80% for black women and near 70% for white women.
You have likely heard of someone who has had fibroids. I want to take a step back and think about the impact of fibroids on women. An important study estimated annual direct costs of fibroids (surgery, hospital admissions, outpatient visits, and medications) were $4.1 to $9.4 billion!!! The study found the total societal costs of fibroids (lost work costs, costs related to treatments, and risks of fertility and pregnancy complications) to be more than costs associated with breast cancer, colon cancer, or ovarian cancer and nearly one fifth of the annual cost of diabetes in the United States.
How do I know if I have fibroids?
Think of fibroids as causing bulk (symptoms caused by the mass effect of an enlarged uterus) or bleeding symptoms. Bulk symptoms include constipation, bloating, early satiety (feelings of fullness), urinary frequency, and sometimes even pain with sex. Bleeding symptoms include heavy bleeding during your menses, sometimes with passage of blood clots. If you’re having some of these symptoms, check in with your OBGYN. We use pelvic ultrasounds as one of the first steps to screen for fibroids.
Do fibroids make it harder to get pregnant?
Fibroids account for 1-2% of infertility. Difficulty getting pregnant will depend on where the fibroids are located. If submucosal or intramural fibroids distort the lining of the uterus, they can impede implantation of an embryo and increase the chance of miscarriage. Have a conversation with your OBGYN about your fibroids when you’re ready to conceive.
If I do get pregnant, is my pregnancy at risk?
Again, it depends on the location and number of fibroids. Sometimes fibroids can degenerate (the tissue starts to die), and this can be very painful. There is a slightly increased risk of preterm labor and preterm birth (0.9%). If fibroids are distorting the shape of the uterus, there is an increased chance of the baby being sideways (transverse) or breech (head up, rather than down). There is also an increased risk of problems with labor; for example, not dilating and possible hemorrhage (too much blood loss) depending on the number and location of fibroids. If you’ve had surgery to remove fibroids (a myomectomy), you may need a cesarean section. This is something that your OBGYN will decide based on the number and/or location of fibroids at time of removal.
How are they treated?
Treatment depends on what symptoms bother you most and whether you desire future pregnancy.
For bleeding symptoms, there are medications (hormonal and non-hormonal options) as well as surgery. Hormonal options include birth control pills, IUDs, Nexplanon, Depo Provera, progestin-only pills (rumor: birth control pills do NOT cause fibroids to grow), or GnRH (Gonadotropin-releasing hormone) agonists (activates the Gonadotropin hormone receptor) like Lupron. Non-hormonal options include Tranexamic acid, a medication that acts as an antifibrinolytic (interferes with the body’s clotting and slows down bleeding).
For bulk symptoms, medications (specifically GnRH agonists like Lupron) can help the uterus and fibroids shrink about 30%.
If you desire future pregnancy and require surgical treatment, then we recommend a myomectomy, a surgery (either open surgery or minimally invasive) that removes JUST the fibroids. We want your uterus to heal after a myomectomy, depending on the location and/or number of fibroids. If you do decide on a myomectomy, make sure to talk to your OBGYN about how long you will need to wait afterwards to get pregnant and if you will need a cesarean section at time of delivery. If you’re done having children or are sure you don’t ever want to be pregnant, then consider an endometrial ablation (a procedure that essentially burns the lining of the uterus), a uterine artery embolization (a procedure that temporizes blood flow to the uterus and can shrink the uterus and fibroids 30-50% in 3-6 months), or a hysterectomy (a surgery that removes the uterus).
There is a LOT of incredible research going into fibroids, minimally invasive treatments, and medications. Talk to your doctor if you have any questions!
Shop Products From This Article
Backed by science, trusted by mothers
We’re glad you’re here—join thousands of happy customers on the journey to parenthood and beyond.
Shop Now






















