What is a Good Beta hCG After an IVF Embryo Transfer?

The beta hCG test is the blood pregnancy test performed after an IVF embryo transfer. The results of this test are predictive of the chances of success for a baby. In this article, we’ll review what the data says about various beta levels.
Human chorionic gonadotropin (hCG) is the first hormonal message from the placenta to the mother. It is called the pregnancy hormone because it is only present during pregnancy and can be detected by early pregnancy tests or a blood test. Beta hCG (aka β-hCG ) is a quantitative serum test (done by your fertility clinic) to determine the level of hCG hormone present in your blood. Serum β-HCG is proportional to the number and activity of the trophoblastic cells, and research shows that a higher serum β-HCG level is associated with pregnancy outcomes and IVF success.
What is a normal hCG level after IVF?
Understanding the basics of IVF is beyond an embryo transfer. hCG levels also play a significant role after IVF. So what is a good hCG level to look out for? There is no single hCG level or cut-off that defines a normal pregnancy. The beta hCG will vary based on the type of embryo you transferred (was it fresh? Frozen?) and when the hCG test is performed. In general, a beta hCG level of over 100 is generally considered a good, positive result. But what's more important than the absolute beta number that helps determine normal levels is the rate of increase over time (it should double every 48 hours). The higher the percentage of rise in hCG drawn two days following the initial beta, the better the chances for success.
What's more important than the absolute beta number is if the number increases substantially over time.
There are usually three beta hCG tests (assuming the first and second are positive). Then, you move onto a vaginal ultrasound at five to eight weeks to look for both a heartbeat and a gestational sac to confirm the pregnancy. This ultrasound is much more predictive of pregnancy outcomes than hCG levels. So, if your first beta is low, do not panic!
What should the hCG level be 12 days after the embryo transfer? 14 days after?
A strong beta number at 17 days after fertilization (14dp3dt or 12dp5dt) would be over 200 mIU/mL (or IU/L, they are equivalent). One study of 523 IVF pregnancies found that betas over 200 IU/L at this time had the greatest chance of success.
In this study, lower serum β-HCG levels were related to higher rates of early pregnancy loss and ectopic pregnancy for women with singleton pregnancies (just one baby). Here is a chart of outcomes based on beta hCG levels:

IVF Transfer Outcome by Beta hCG Level on Day 14. Data from a study of 523 pregnancies after IVF fertility treatment.
What can beta HCG levels tell you?
Can beta HCG levels after IVF predict miscarriage?
Unfortunately yes. A study of 177 IVF cycles showed that pregnancies with a beta hCG concentration <85 mIU/mL at Day 13 had an 89% risk of having a first trimester miscarriage, and pregnancies with β-hCG >386 mU/mL had a 91% chance of a live birth.
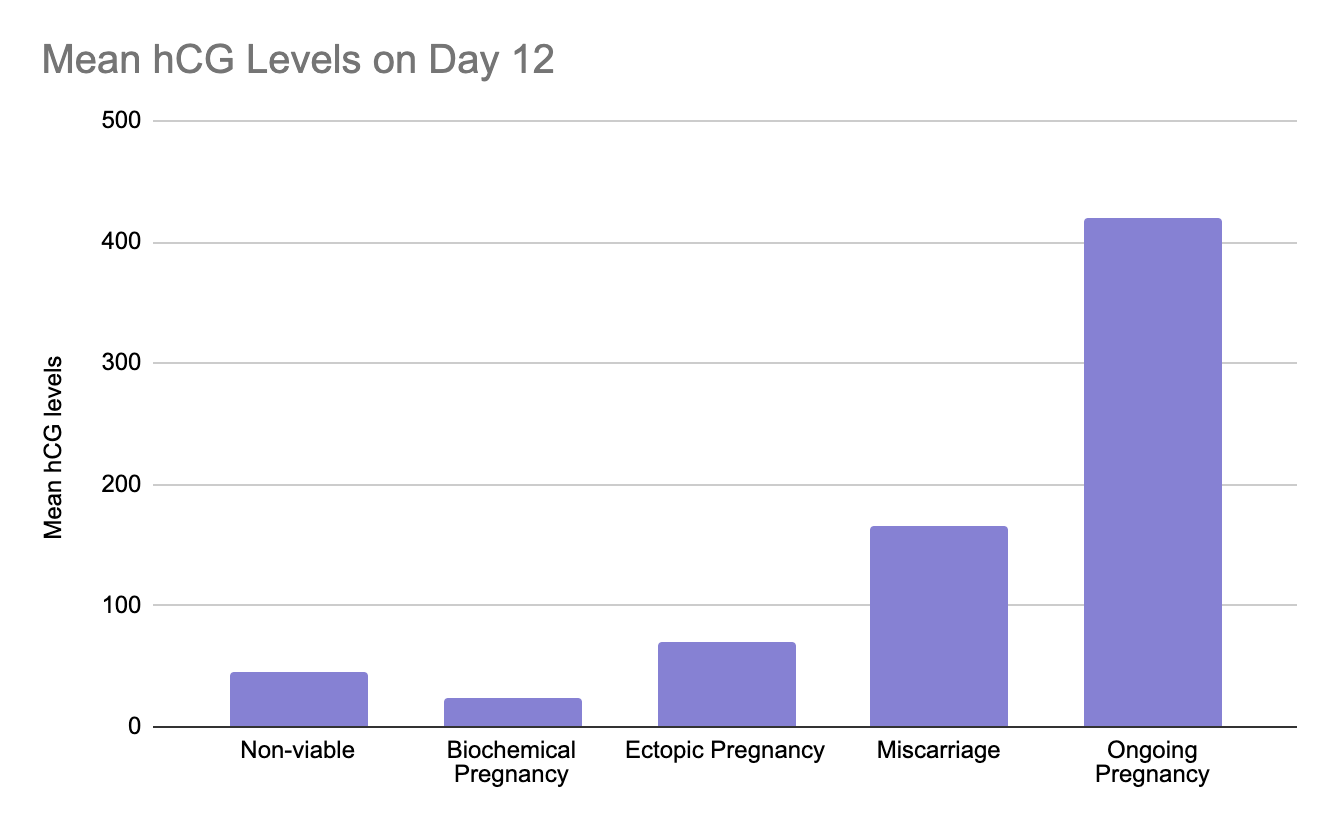
Data from a study of 123 IVF participants. Beta hCG levels were taken 12 days after an embryo transfer.
What does a high beta hCG mean?
A high beta hCG could indicate multiples (twins or triplets), which would be confirmed through an ultrasound. One study found that median hCG levels on Day 13 after a fresh embryo transfer were 329 for women with one baby and 544 for women carrying twins.
There are other medical reasons that could be behind an unusually high beta hCG. If there’s any concern about a high hCG level, your doctor will review the test results and discuss the next steps.
What does a low beta hCG mean?
Even though the data of outcomes from low beta hCG levels looks scary, remember that there are many normal, healthy pregnancies that start out with a low beta hCG. It A low hCG level could mean the embryo has a slower implantation process. Try not to obsess too much with the hCG numbers. As stated above, the ultrasound findings are much more predictive of pregnancy outcomes than the hCG levels. If you have concerns about your beta hCG numbers, always talk to your doctor. Don’t be afraid to ask them what they think is going on and what your chances are of success given the information at hand.
Can beta hCG levels predict singleton or twins?
Yes, multiple pregnancies (twins, triplets, etc.) have significantly higher hCG levels compared to singletons.
One study broke out twin pregnancies and found that a beta HCG on day 13 after an embryo transfer of <207 mIU/mL had a 33% chance of delivering twins and a 55% risk of having a vanishing twin. The study showed that twin pregnancies with a beta hCG ≥768 mIU/mL had an 81% chance of delivering live twins and a 19% risk of having a vanishing twin (there were no pregnancy losses in this group).
What if beta hCG is not rising or doubling?
If your hCG is rising, but not doubling, it doesn’t necessarily mean that something is wrong. Some recent studies have shown that the rise could be as slow as 53% in two days and the pregnancy could still turn out to be normal. Talk to your doctor about the numbers and what they mean given your situation.
However, if your hCG level is falling, it is likely that the implantation was not successful. Your doctor will have you take additional blood tests until hCG is no longer detected to ensure that you have recovered and can move forward. If your hCG stays the same and does not drop to zero, your doctor will talk to you about options to intervene.
A failed transfer is devastating. Read more about Strategies to Cope During Fertility Treatments.
Is it true that girl embryos have higher beta hCG?
One international study found the average beta hCG value was higher for female fetuses compared to males, but the results were not statistically significant. Another study found that gender-related difference inHCG does exist as early as three weeks after fertilization, but that the difference is not strong enough to be used to predict fetal sex"because of the small proportion of pregnant women with serum HCG concentrations that are high or low enough to allow a prediction with high probability".
Beta hCG may not be reliable for women with ovarian hyperstimulation syndrome (OHSS)
For women with ovarian hyperstimulation syndrome (OHSS), hCG levels may fluctuate abnormally. This is because fluid build-up from OHSS could dilute the blood levels. Although this happens, the good news is that research shows that the outcomes of these pregnancies remained comparable to those of IVF pregnancies without OHSS. Another study even showed that there is a lower rate of early miscarriage in the OHSS group (7.8%) than overall (16%).
What are normal hCG results throughout pregnancy?
hCG level rises rapidly during the first trimester and then declines slightly. Here are the expected hCG ranges in the first 18 weeks of pregnancy:
-
3 weeks: 5 - 72 mIU/mL
-
4 weeks: 10 -708 mIU/mL
-
5 weeks: 217 - 8,245 mIU/mL
-
6 weeks: 152 - 32,177 mIU/mL
-
7 weeks: 4,059 - 153,767 mIU/mL
-
8 weeks: 31,366 - 149,094 mIU/mL
-
9 weeks: 59,109 - 135,901 mIU/mL
-
10 weeks: 44,186 - 170,409 mIU/mL
-
12 weeks: 27,107 - 201,165 mIU/mL
-
14 weeks: 24,302 - 93,646 mIU/mL
-
15 weeks: 12,540 - 69,747 mIU/mL
-
16 weeks: 8,904 - 55,332 mIU/mL
-
17 weeks: 8,240 - 51,793 mIU/mL
-
18 weeks: 9,649 - 55,271 mIU/mL
IVF fertility treatment can be an amazing way to grow a family. I know—I would not be a mother today without IVF. But it also comes with emotional ups and downs.
Up next:
Reach Out, We're Here
Have questions about your order or products? For the speediest answer, check out our FAQ section. Need something else? Come find us below.
Please keep in mind our regular business hours; Monday-Friday, 9am-5pm CT.
Customer Support
support@natalist.com
Press Inquiries
media@everlyhealth.com
Business & Partnerships
team@natalist.com
Affiliates + Influencers
team@natalist.com
Job Openings
Careers Page
























